Afex Incontinence Management System for Men
Our mission is to improve the quality of life and care for people around the world by developing and commercializing innovative products and transformational technologies for healthcare. Since 2002, our mission-focused determination has guided us to develop patented and proprietary medical devices that offer significant benefits to patients and caregivers who use our products every day. Our current brands offer patients access to innovative products and technologies for management of incontinence, bladder leakage, and other urinary management needs.
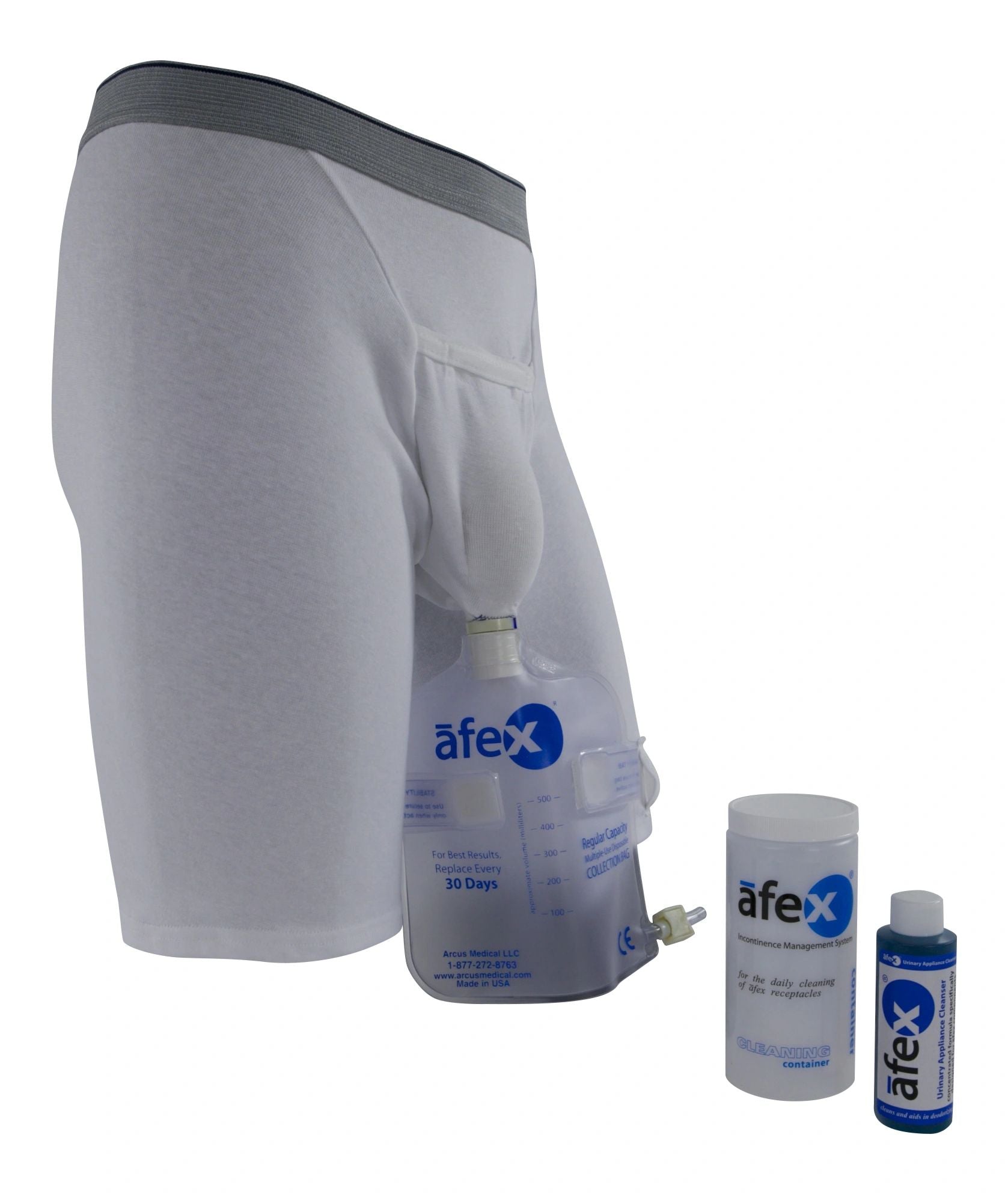
Afex® provides superior daytime protection with its patented receptacle and direct-connect collection bag. The receptacle and bag is discreetly supported by a comfortable, specially designed cotton brief or supporter. Patients who use our Afex® system enjoy the benefits of an innovative product that effectively controls odor, leakage, and wetness often associated with other male incontinence products.

How to choose your KIT
Click Here to see Chart






Afex Active Starter Kit
The standard Afex® Active Starter kit contains everything you need to begin using Afex®. It includes:
- 1 full brief - sports active style
- 1 high style receptacle
- 1 standard 500 ml collection bag
- 1 cleaning container 4 oz bottle of liquid cleanser concentrate
Please specify your brief waist size. The high style receptacle is recommended for active and night use. Low style receptacle is generally recommended for more sedentary or mobility assisted use.
Healthcare Provider Perspective
Prostate issues are a common cause of male incontinence symptoms. An enlarged prostate, known as Benign Prostate Hyperplasia (BPH), is more common among older men and BPH can cause varying levels and types of male incontinence. In the video below, Dr. Ryan Barnes from Virginia Urology in Richmond, Virginia talks about BPH, its symptoms, what causes it and how it is treated. Enlarged prostate or Benign Prostatic Hyperplasia (BPH) affects over 17 million men in the U.S. according to Virgina Urology. You can visit Virginia Urology at www.uro.com.